If you struggle to beautifully and reliably restore cervical lesions, your’e not alone! Non-carious cervical lesions appear simple and straightforward to restore but can present a significant challenge for many clinicians.
The restorative challenges these pose are:
- Access to the lesion
- Moisture control
- Correct placement of restorative material
- Contour management
- Marginal integrity
- Patient discomfort
- Chair time
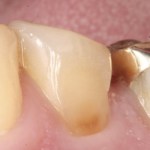
 Cervical lesions are generally caused by abrasion forces, abfraction, acid erosion and previously treated caries (Borcic, Anic, Urek, & Ferreri, 2004). The nature of the lesion usually implies the patient has acute symptoms of dentine hypersensitivity, but can easily become pulpally involved.
Cervical lesions are generally caused by abrasion forces, abfraction, acid erosion and previously treated caries (Borcic, Anic, Urek, & Ferreri, 2004). The nature of the lesion usually implies the patient has acute symptoms of dentine hypersensitivity, but can easily become pulpally involved.
The old way: direct composite cervical restorations
Resin composites appear to be the best used because they offer excellent colour stability, anatomical form and texture. But achieving marginal integrity intra-orally is quite difficult!
Moisture control; a big challenge with composites! A rubber dam or retraction chord usually involves the need for Local Anesthesia (LA) which increases surgery time and patient discomfort. A clamp can also cause soft tissue scarring and eventually gingival recession.
The new way: direct-indirect cervical restorations
 The direct-indirect class V restorative method aims to minimise the challenges and difficulties mentioned above (Newton, 2015).
The direct-indirect class V restorative method aims to minimise the challenges and difficulties mentioned above (Newton, 2015).
The composite resin is applied and sculpted directly on the tooth surface prior to using any etch or adhesives. It is then light cured and finished extra-orally prior to placement. The research points to increased physical material properties, greater operator control over the anatomy and colour and indications for anterior and posterior lesions (Fahl Junior, 1996).
Shaping and polishing is done extra-orally and allows greater clinical control with reduced chances of causing iatrogenic ledges, overhangs and rough margins.
The restoration is only bonded intra-orally after contouring, shaping and refining and thus there is a lower risk of exposure to gingival tissue fluid or saliva.

The method
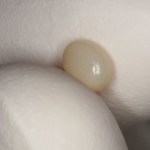
- Following basic moisture isolation, composite is rolled into a ball and pressed onto the lesion surface using digital pressure. It should cover not just the cavity but extended beyond the margins over the free gingival margin.
- Instruments can be used for refinement but often un-necessary.
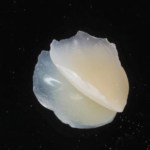
- The composite is then light cured and removed.
- The margins are clearly visible but can also be outlined using a pencil for clear visualisation. Finishing is completed with discs.
- The restorative fit surface can be air-abraded for better bond strength.
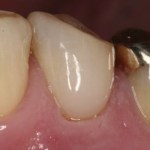
- It can then be cemented just as you would any composite inlay/veneer.
The references below include the article from which this technique was introduced! Read it for more pictures and more details! The author also uses pink composite to mimic gingival tissue in cases where an extended crown height appearance is undesirable.
References
Borcic, J., Anic, I., Urek, M. M., & Ferreri, S. (2004). The prevalence of non-carious cervical lesions in permanent dentition. Journal of Oral Rehabilitation, 31(2), 117–123.
Fahl Junior, N. (1996). The direct/indirect composite resin veneers: a case report. Practical Periodontics and Aesthetic Dentistry : PPAD, 8(7), 627–38; quiz 640.
Newton, F. J. (2015). Direct-Indirect Class V Restorations : A Novel Approach for Treating Noncarious Cervical Lesions, 27(5), 267–284. https://doi.org/10.1111/jerd.12151
Images used were presented in the above referenced article